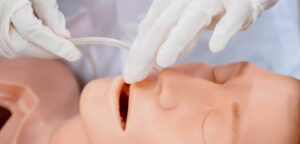
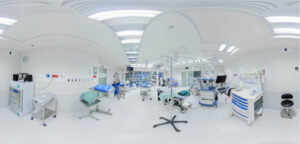
Dynamic Simulations for Teaching
Computers have made it easier for instructors to use simulations in their teaching. These are usually self-paced and fully automated, allowing the instructor to step back and watch students work. But this automation tends to illuminate the randomness and sudden changes that happen in a